Abstract
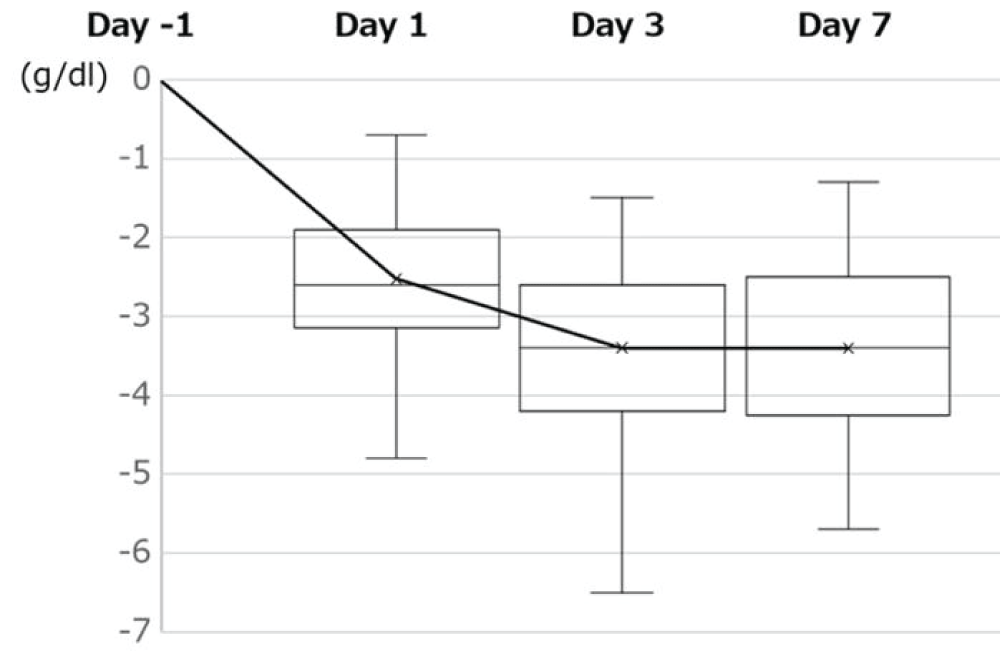
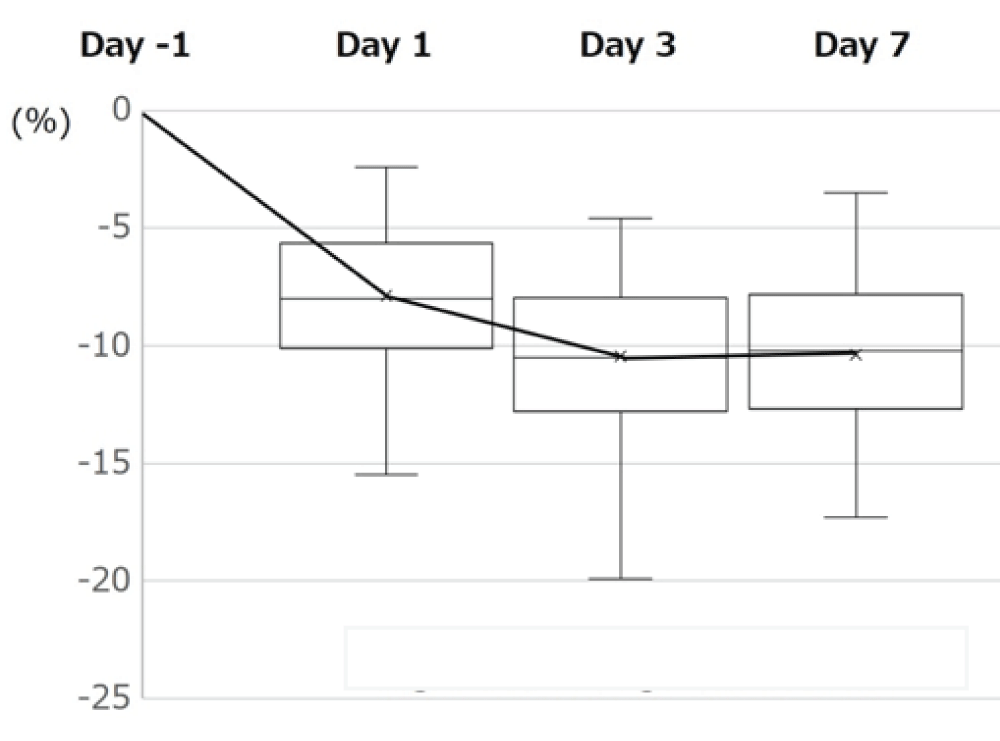
Background: Recently, the amount of bleeding during and after Total Hip Arthroplasty (THA) has decreased owing to the use of tranexamic acid, advancements in surgical devices, improvements in surgical skills, and the introduction of minimally invasive surgery. Therefore, the need for blood transfusions is decreasing. We monitored haemoglobin (Hb) and haematocrit (Ht) levels, estimated blood loss, transfusion rates, and other aspects of Anterolateral Supine THA (ALS-THA) performed at our institution without autologous blood donation and closed suction drainage.
Methods: Patients (n = 316) with preoperative Hb ≥10.0 g/dL during primary unilateral THA performed at our hospital from May 2021 to July 2023 were included. Hb and Ht levels, surgical time, intraoperative blood loss, estimated postoperative blood loss, allogeneic blood transfusion rates, and complication rates were evaluated. We performed logistic regression analysis on age, sex, blood type, height, weight, BMI, preoperative Hb, and preoperative Ht to evaluate the risk of blood transfusion. Receiver Operating Characteristic (ROC) analysis was performed on preoperative Hb levels and blood transfusions.
Results: Blood transfusions were performed in 10 of the 316 cases (3.2%), with a transfusion rate of 16.7% in patients with preoperative Hb < 12g/dL.
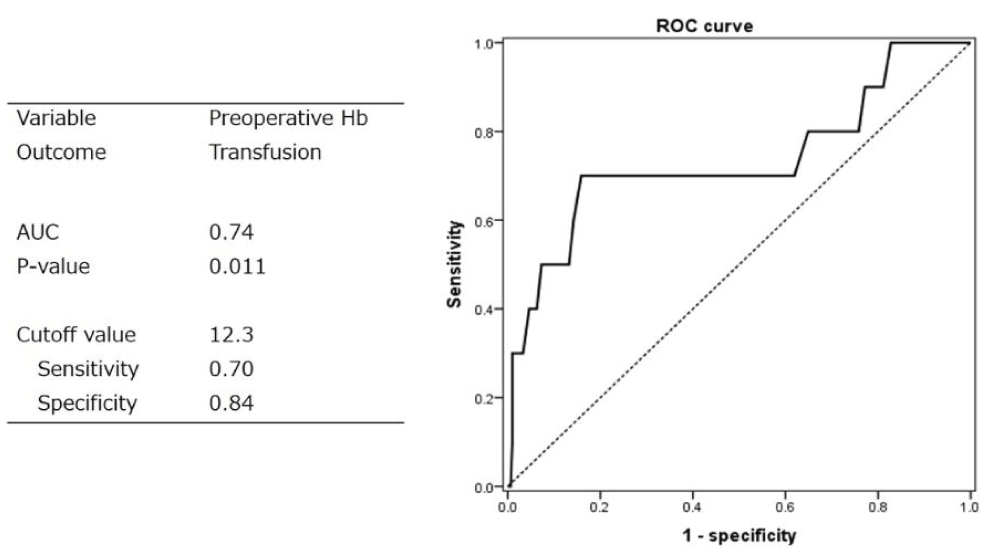
Univariate analysis revealed significant differences in preoperative Hb and Ht levels, whereas multivariate analysis showed a significant difference in preoperative Hb (odds ratio 0.39). In ROC analysis, the cutoff value was Hb 12.3 g/dL (sensitivity 0.7; specificity 0.84).
Conclusion: The preoperative Hb level was the most important factor contributing to the transfusion risk in THA. Preoperative anemia treatment may further reduce blood transfusions.